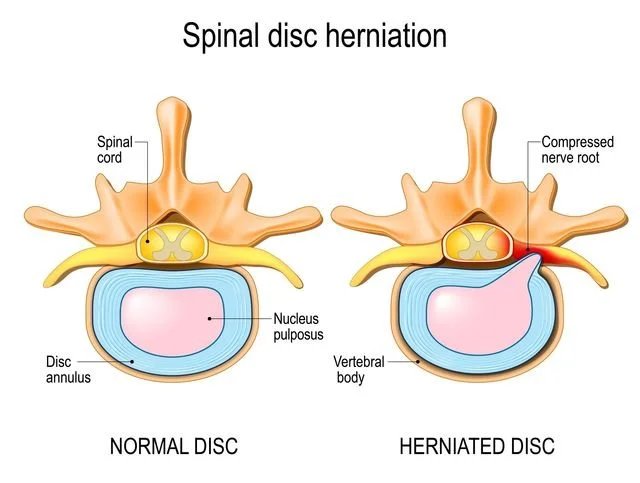
Disc Bulge vs. Disc Herniation
Low back and neck pain are among the most common reasons people seek medical care. When imaging studies like MRI are performed, patients are often told they have a “disc bulge” or a “disc herniation.”
While these terms are frequently used interchangeably in casual conversation, they describe very different structural changes within the spinal disc. Understanding the distinction is important because the mechanism of injury, symptom patterns, and treatment strategies can vary significantly.
In this article, we’ll break down:
The anatomy of a spinal disc
The difference between a disc bulge and a disc herniation
How these injuries occur
Why spinal biomechanics play a major role
How chiropractic care can help address the root cause
The Anatomy of the Spinal Disc
Between each vertebra in the spine sits a spinal disc, which functions as both a shock absorber and a motion stabilizer.
Each disc has two main components:
Annulus Fibrosus
The tough outer ring made of layered collagen and elastin fibers.
Nucleus Pulposus
The soft, gel-like center that distributes pressure across the spine.
Under normal conditions, the disc allows the spine to bend, twist, and absorb load while maintaining stability. But when forces on the spine become uneven or excessive, the disc can begin to deform.
What Is a Disc Bulge?
A disc bulge occurs when the disc begins to extend outward beyond the edges of the vertebra, but the outer fibers of the annulus remain intact.
Think of it like:
A tire that is slightly overinflated and bulges outward.
The disc wall has not torn — it has simply lost its normal shape.
Key Characteristics of a Disc Bulge
The annulus fibrosus remains intact
The disc protrudes symmetrically or broadly
Develops gradually over time
Associated with degeneration or chronic mechanical stress
Many disc bulges are asymptomatic, but if the bulge presses on nearby nerve structures, it can produce symptoms such as:
Localized back or neck pain
Stiffness
Muscle spasms
Occasionally nerve irritation
What Is a Disc Herniation?
A disc herniation occurs when the outer fibers of the annulus tear, allowing the inner nucleus material to push outward. Disc herniations are caused by a single trauma or multiple microtraumas.
In more severe cases, the nucleus can even extrude beyond the disc entirely.
This is why herniations often produce more dramatic symptoms.
Key Characteristics of a Disc Herniation
Annular tear is present
Inner disc material protrudes outward
Often asymmetrical
More likely to irritate or compress spinal nerves
Common symptoms include:
Radiating arm or leg pain
Numbness or tingling
Muscle weakness
Shooting nerve pain
For example:
A lumbar disc herniation may produce sciatic pain down the leg, while a cervical herniation may cause symptoms into the shoulder or arm.
How Do Disc Injuries Happen?
Disc injuries typically happen in two ways. Chronic stress over time, disc bulge, or a traumatic event, disc herniation. Bulged discs are more likely to herniate as they are already in a compromised position.
1. Repetitive Improper Spinal Mechanics
When spinal joints move improperly — whether due to posture, muscle imbalance, or joint restriction — forces on the disc become unevenly distributed.
Over time, this can cause the disc to:
weaken
deform
eventually tear with trauma
Poor biomechanics can come from:
prolonged sitting
forward head posture
improper lifting mechanics
athletic overuse
2. Sudden Load or Trauma
Disc herniations occur when the spine experiences a sudden increase in pressure, such as:
lifting heavy objects
twisting while bending
sports injuries
car accidents
If the disc is already weakened, even a relatively small movement can cause the annulus to tear.
3. Degenerative Changes
As we age, discs naturally lose water content and elasticity. This process, called disc degeneration, makes them more vulnerable to bulging or herniation under stress.
However, degeneration alone does not determine symptoms — mechanical stress patterns still play a major role.
Why Spinal Biomechanics Matter
One of the most overlooked aspects of disc pathology is how the spine moves.
Even a small joint restriction can alter motion patterns across multiple segments of the spine. When certain areas stop moving normally, other segments must compensate.
This leads to:
abnormal loading of discs
increased shear forces
accelerated wear of spinal structures
Over time, these dysfunctional movement patterns can contribute to both disc bulges and herniations.
This is why simply treating pain without addressing underlying spinal mechanics often leads to recurring symptoms.
How Chiropractic Care Can Help
Chiropractic care that focuses on restoring normal spinal motion and biomechanics is essential.
Rather than only masking symptoms, the goal is to reduce the mechanical stress that contributed to the injury in the first place.
Restoring Joint Motion
Chiropractic adjustments help restore movement in restricted spinal joints.
When motion is normalized:
pressure distribution improves
disc stress is reduced
surrounding muscles relax
Reducing Nerve Irritation
When discs irritate nearby nerves, inflammation and muscle guarding can worsen symptoms.
Improving spinal mechanics can help decrease mechanical irritation on nerve structures and allow the body to heal.
Improving Spinal Stability
Chiropractic care often incorporates:
postural correction
spinal stabilization exercises
ergonomic guidance
These strategies help patients maintain healthier movement patterns, preventing further disc stress.
The Big Picture
Disc bulges and disc herniations represent different stages of disc injury, but both are heavily influenced by how the spine moves and distributes force.
Understanding the mechanical component of spinal health is key.
When spinal biomechanics are addressed, many patients experience:
reduced pain
improved mobility
decreased nerve irritation
better long-term spinal health
The goal is not simply to treat the disc itself — but to restore the functional integrity of the spine as a whole.
Dr. Frank Berzanskis Jr., D.C.
Trauma Qualified
ScoliBrace Certified
ScoliBalance Certified